The Knee Joint
The knee joint has often been thought of as simple hinge joint however, the motion at the knee due to its structure of articulating surfaces between the femur and tibia (thigh bone and lower leg bone) we often see the resulting motion of rolling, sliding and spinning at the joint. Meaning that we get motion in all three joint planes however, the majority is seen between flexion and extension or bending and straightening of the knee.
The Ligaments of the Knee
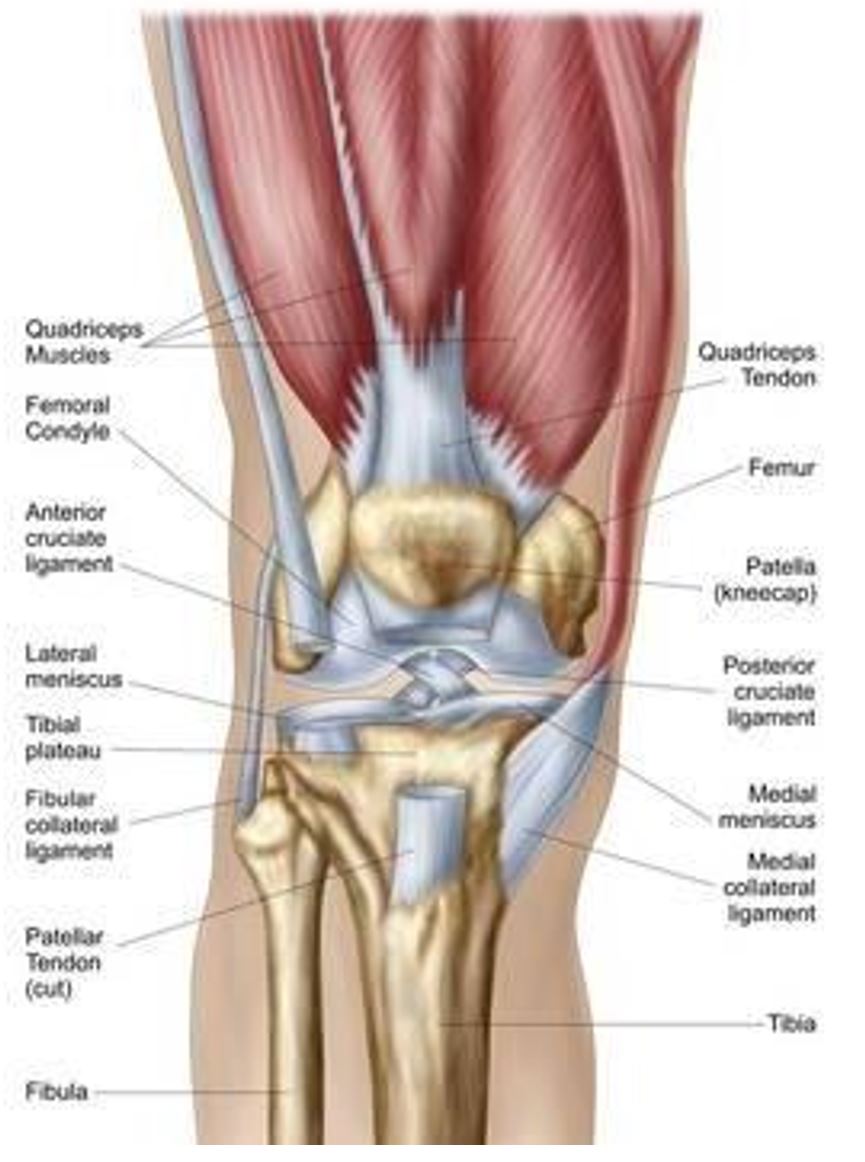
The ligaments of the knee are made of dense extremely strong bands of collagen fibers and the orientation of the fibers are responsible for their behaviours. Almost all fibers are arranged in parallel bundles and have the ability to withstand strong tensile loads. The main four ligaments of the knee consist of the anterior cruciate ligament, the posterior cruciate ligament, the medial and lateral collateral ligaments.
The Role of Ligaments / Joint Capsule
The role of the ligaments is to prevent abnormal movement and motion in the knee – they are there to stabilise the knee whilst controlling and directing normal knee movement. Each ligament has a particular role and responsibility, when one of these structures is damaged it can result in excessive motion leading to further internal damage on the knee from excessive load and abnormal motion.
The Role of the Anterior Cruciate Ligament (ACL)
A key ligament in the passive stability of the knee is that of the Anterior Cruciate Ligament (ACL) – The role of this cruciate ligament is a primary restraint to anterior displacement of the tibia (the lower leg bone moving too far forward under the thigh bone). It also acts as a secondary restraint of internal tibial rotation (the shin bone rotating towards the midline) and a very minor role in restraint of varus and valgus deformities (the lower leg bone kicking towards or away from the midline of the body.)
The anatomy of the ligament and its fiber bundles do not function as a simple band of fibers under constant tension but rather have different patterns of tension through the knees full range of motion. It has two distinct parts;
1. A large ‘anteromedial band’ which is taught in flexion and relaxed in extension – this band is responsible for limiting anterior translation of the tibia on the femur.
2. A small ‘posterolateral band’ which is taught in extension and relaxed in flexion – limits anterior translation of the tibia on femur & internal rotation of the tibia on the femur.
Due to its structure it has a functional restraining role throughout the whole continuum of motion and influences the knee in all joint positions.
While the knee relies heavily on the ACL as well as the surrounding ligaments and capsule for its stability and guidance of motion the supporting dynamic stabilisers of the knee are also crucial to the knees function. Muscles such as our hamstrings, quadriceps, Illiotibial band, gastrocnemius and popliteus muscles must work together with our bodies mechanoreceptors (neural tissue which tells our brain where our limb / joint is in space) to ensure the complete function and stability of the knee.

Injury to the ACL – How does it Happen?
Anterior Cruciate injury can be one of the most debilitating knee injuries physically and psychologically to athletes of all participation levels. However, it is not just limited to athletes and sports people but can also effect workers in any occupation.
Anterior Cruciate Ligament rupture or strain can occur in contact and non-contact environments. It is hypothesised that 80% of ACL injuries occur in a non-contact environment more particularly during deceleration type movements these most commonly include;
Jumping, cutting and side stepping as well as rotation on a fixed foot such including movements such as landing then changing direction. Impact and collision ACL ruptures usually occur from a blow to the outside of the knee turning the knee towards the midline of the body. It is common for the injured individual to report a ‘POP’ and develop swelling and bleeding within the knee joint in minutes to hours. Individuals are usually unable to weight bear have a loss or range of motion and a general feeling of instability or ‘giving way’ within the knee. There is also potential to injure surrounding structures commonly termed ‘the unhappy triad’ which entails injury to surrounding meniscus (cartilage) and the medial collateral ligament.

Initial Treatment of the Injury
Initial treatment of the injury usually consists of compression to reduce inflammation, ice, crutches to allow mobilisation and very gentle mobilisation exercises.
It is important to be assessed by a trained individual who can perform a sound clinical and subjective assessment of the individual and injury – allowing for rapid recognition and intervention steering the individual towards the pathway to orthopaedic assessment for evaluation. MRI is used to confirm ACL rupture and any other surrounding tissue damage.
The Role & Importance of seeing an Orthopaedic Specialist
Your Orthopaedic surgeon will assess and recommend a tailored approach to your surgery and graft choice – depending on your individual history, as there are many options available each with their own advantages and disadvantages from a short and long term perspective.
Currently, single hamstring techniques are an option for ACL reconstructions where technology and techniques have allowed the use of 1 hamstring instead of 2 to create the strength needed to reconstruct the ligament and that the 1 hamstring achieves a size closer to a native ACL than 2 hamstring techniques. Single hamstring graft selection is the most common practice and has the best supporting current evidence. The surgeons preferred method will determine which portals are drilled for insertion and alignment of the ACL graft however, the preferred current method with the most accuracy revolves around using a ‘Through Portal Technique’. Your orthopaedic specialist will be able to discuss your options with you coming up with a suitable option with anticipated maximal results.
Post-Operative Care & Rehabilitation for Anterior Cruciate Ligament Reconstruction
Physiotherapy care for ACL reconstruction should start day one postoperatively with early mobility and weightbearing shown to prevent patellofemoral pain & stiffness in the knee while possibly preventing arthrofibrosis (scar tissue build up) in the knee.
The rehabilitation process can be broken up into 6 stages. Each stage pertains to the healing phase of the graft, account for any other surgery that has been performed in conjunction with the ACL repair and if the patient is meeting the goals and outcomes set during each stage of the rehabilitation plan, hence the plan is tailored based on the surgery and the patient’s individual progression and desired post-operative pre-injury goals.
